Tick Paralysis in Dogs
Understand the dangers of tick paralysis in dogs, from early warning signs to life-saving treatments and prevention strategies for pet safety.
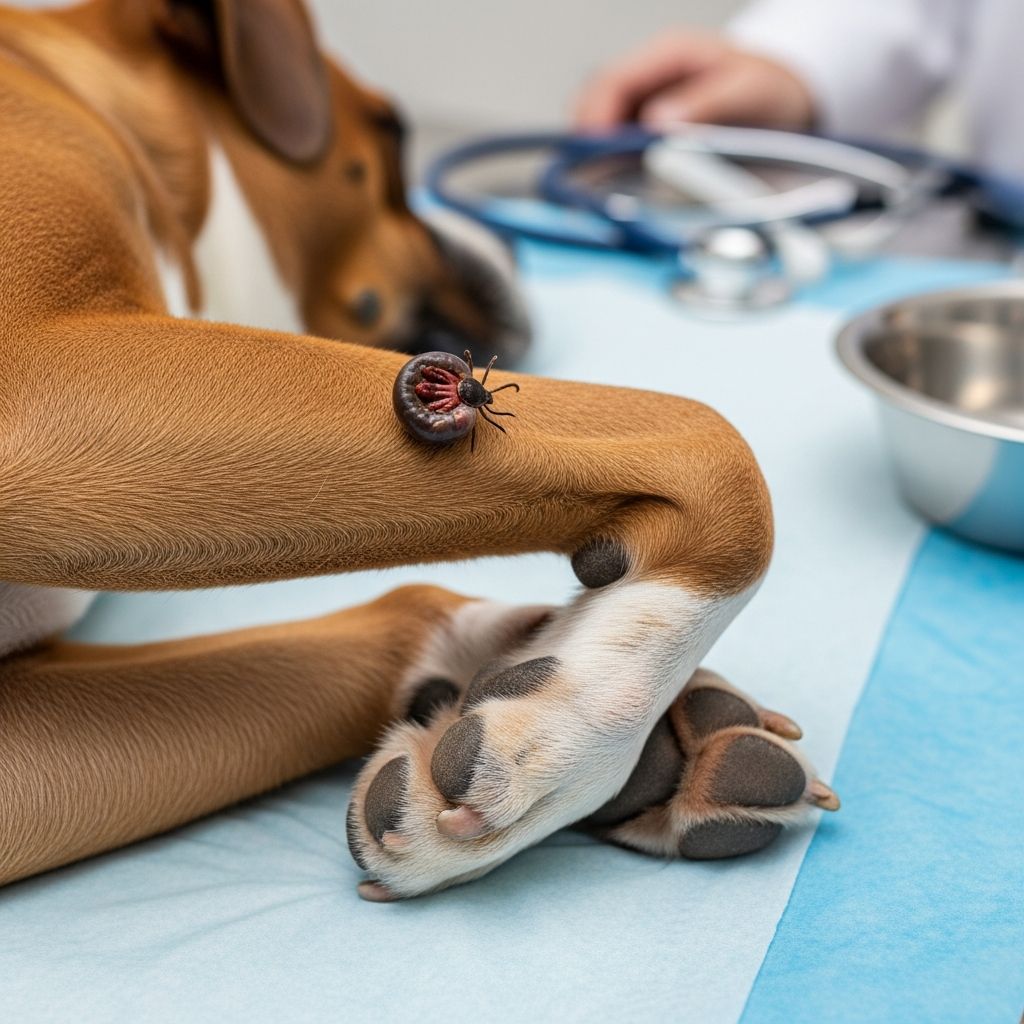
Tick Paralysis in Dogs: A Rising Threat to Canine Health
Tick paralysis represents a severe neurological condition in dogs triggered by toxins from certain tick species. These parasites inject neurotoxins through their saliva during feeding, leading to muscle weakness that ascends from the legs upward, potentially causing respiratory failure if untreated. Prompt detection and intervention are critical, as symptoms can progress rapidly even after tick removal in some cases.
Understanding the Science Behind Tick Toxins
The primary culprits are ticks like the Australian paralysis tick (Ixodes holocyclus) and North American species such as the Rocky Mountain wood tick and American dog tick. Female ticks, especially engorged ones, release potent neurotoxins that disrupt nerve signal transmission, mimicking a flaccid paralysis without inflammation. Attachment for at least 3-7 days is typically required before symptoms manifest, emphasizing the need for daily checks in tick-prone areas.
Unlike infectious diseases, this condition stems purely from toxin accumulation. In regions with high tick prevalence, such as coastal Australia or wooded U.S. areas, incidence peaks during warmer months. Veterinary data indicates that without intervention, mortality can reach high levels due to respiratory collapse.
Early Detection: Spotting Subtle Signs First
Initial symptoms often mimic mild illness, delaying diagnosis. Dog owners should watch for:
- Reduced appetite and lethargy, signaling toxin onset.
- Altered bark or voice changes from laryngeal muscle impact.
- Mild hind leg wobbling or coordination loss during walks.
- Urinary hesitation or incontinence as nerves weaken.
These mild indicators can escalate within 24-48 hours post-tick attachment. Regular grooming reveals ticks in hidden spots like ears, armpits, or paw pads.
Progression to Moderate and Severe Stages
As toxins build, paralysis intensifies. Moderate cases feature pronounced leg weakness, standing difficulties, and respiratory strain with grunting or noisy breaths. Dogs may retch, risking aspiration pneumonia from frothy vomit.
Severe manifestations are emergencies: complete inability to stand, labored breathing, facial droop, dilated pupils, and gagging. Respiratory muscles fail, leading to exhaustion and potential cardiac complications like arrhythmias. Prognosis worsens with inspiratory dyspnea, crackles, or vomiting.
| Stage | Key Symptoms | Timeframe |
|---|---|---|
| Mild | Lethargy, voice change, slight weakness | Days 3-5 post-attachment |
| Moderate | Leg instability, breathing effort, retching | 24-48 hours progression |
| Severe | Full paralysis, respiratory failure, pneumonia risk | 1-5 days untreated |
This table outlines progression, highlighting urgency.
Immediate Response: What to Do If You Suspect Tick Paralysis
Never delay: remove visible ticks with fine-tipped tweezers, grasping close to the skin to extract mouthparts fully, as residual glands may continue toxin release. Rush to a vet even if symptoms seem minor—toxin effects linger up to 24 hours post-removal for certain species.
At the clinic, expect a thorough exam. Vets perform full-body clipping under anesthesia to uncover hidden ticks, especially in furred areas.
Comprehensive Veterinary Treatment Protocols
Treatment combines toxin neutralization and supportive care:
- Tick Antiserum (TAS): Administered IV, it binds toxins; improvement often begins 6-12 hours later.
- IV Fluids: Maintain hydration and support organ function.
- Oxygen Therapy: Nasal or intubation for dyspnea; critical in severe cases.
- Sedation/Anesthesia: Eases breathing, allows suctioning of secretions, and clipping.
- Anti-nausea and Antimicrobials: Prevent vomiting, pneumonia; broad-spectrum antibiotics if aspiration suspected.
- Monitoring: 24-hour ICU with blood tests, X-rays, urinary catheters.
For cardiac issues, medications like verapamil may stabilize heart rhythm. Costs range $900-$2000 for standard cases, higher for ICU stays.
Recovery Timeline and Home Care Essentials
With all ticks removed and TAS given, most dogs recover in 24-72 hours, though severe cases take 2-4 days or longer. Full mobility returns gradually; provide a quiet, stress-free space with soft bedding.
- Assist with feeding and hydration initially.
- Express bladder manually if needed.
- Apply tick preventives post-recovery.
- Monitor for relapse; recheck skin daily.
A small percentage face poor outcomes, prompting humane euthanasia discussions if breathing fails despite support.
Prevention Strategies: Keeping Ticks at Bay
Proactive measures slash risk:
- Daily Checks: Comb fur after outdoor time, focusing on head, neck, groin.
- Preventives: Monthly oral/topical products kill ticks before toxin injection.
- Environmental Control: Mow lawns, avoid brushy areas during peak season.
- Grooming: Short clips in high-risk zones aid detection.
Vaccines aren’t available, so vigilance is key. Consult vets for region-specific advice.
Risks in High-Prevalence Areas
Coastal or forested regions see spikes; puppies, seniors, and overweight dogs fare worse due to resilience gaps. Climate change extends seasons, heightening exposure.
FAQs on Tick Paralysis in Dogs
What is the first sign of tick paralysis in dogs?
Hind leg weakness or wobbling often appears first, followed by voice changes.
Can tick paralysis kill a dog?
Yes, untreated cases lead to respiratory failure and death in 1-5 days.
How long after tick removal do symptoms improve?
24 hours typically, but TAS accelerates to 6-12 hours; monitor closely.
Is tick paralysis contagious?
No, it’s toxin-based, not infectious.
What if no tick is found?
Treat presumptively if symptoms match; hidden ticks are common.
Long-Term Outlook and When to Seek Help
Survivors rarely suffer lasting effects if treated promptly. Annual vet checkups and preventives ensure ongoing protection. If paralysis recurs, investigate underlying issues.
(Word count: 1678)
References
- Tick Paralysis Treatment – Pittwater Animal Hospital — Pittwater Animal Hospital. Accessed 2026. https://pittwateranimalhospital.com.au/tick-advice/tick-paralysis-treatment/
- Paralysis Ticks in Dogs: Symptoms, Treatment, and Prevention Tips — YouTube (Veterinary Channel). Accessed 2026. https://www.youtube.com/watch?v=k8GEj7ns1j8
- Tick Paralysis in Animals – Nervous System — MSD Veterinary Manual. Accessed 2026. https://www.msdvetmanual.com/nervous-system/tick-paralysis/tick-paralysis-in-animals
- Tick Paralysis in Dogs — PetMD. Accessed 2026. https://www.petmd.com/dog/conditions/infectious-parasitic/tick-paralysis-dogs
- Tick Paralysis — American Lyme Disease Foundation. Accessed 2026. https://aldf.com/tick-paralysis/
- Tick Paralysis – CDPH — California Department of Public Health (.gov). Accessed 2026. https://www.cdph.ca.gov/Programs/CID/DCDC/Pages/TickParalysis.aspx
Read full bio of medha deb