Managing Feline Stomatitis: Guide To Treatment And Recovery
Comprehensive guide to understanding, diagnosing, and effectively treating painful mouth inflammation in cats for improved quality of life.
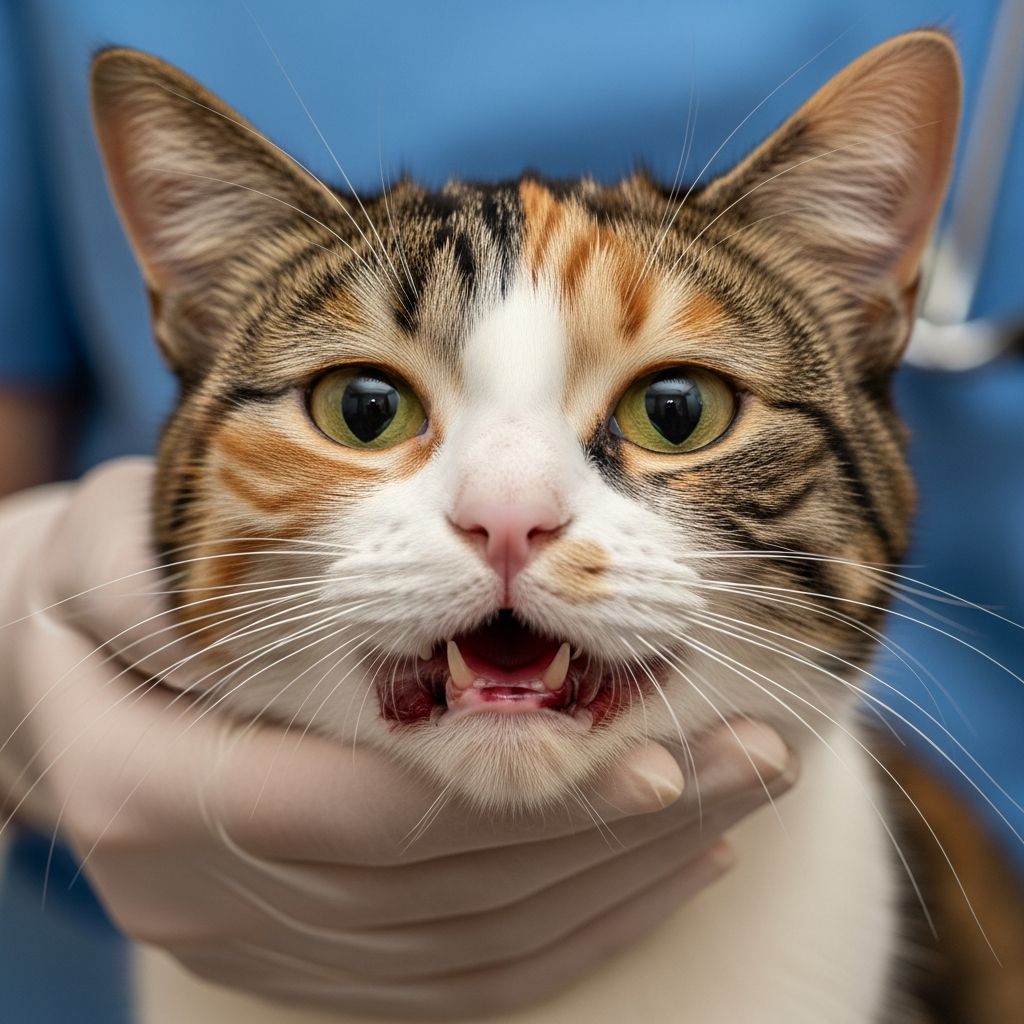
Managing Feline Stomatitis
Feline stomatitis is a debilitating condition causing severe inflammation throughout a cat’s mouth, often leading to pain, difficulty eating, and weight loss. The primary treatment involves dental extractions to remove problematic teeth, achieving remission in most cases.
Understanding the Nature of Feline Stomatitis
This chronic inflammatory disease affects the oral mucosa, gums, and sometimes beyond, distinguishing it from simpler gingivitis. Unlike basic plaque buildup, stomatitis triggers an overzealous immune response, potentially linked to viral infections like calicivirus or bacterial biofilms on teeth.
Cats of any age can develop it, though middle-aged and senior cats are more prone. The inflammation creates painful ulcers and swelling, making normal activities like grooming or eating torturous. Early recognition is crucial, as untreated cases lead to dehydration, malnutrition, and systemic health decline.
Recognizing Key Symptoms in Your Cat
Owners often notice subtle changes escalating to obvious distress. Common signs include:
- Excessive drooling or blood-tinged saliva
- Refusal to eat dry food, progressing to wet food aversion
- Bad breath (halitosis) and pawing at the mouth
- Weight loss despite normal appetite initially
- Difficulty grooming, leading to unkempt fur
- Behavioral shifts like hiding, aggression when touched near the face, or vocalizing in pain
These symptoms overlap with dental disease, but stomatitis features widespread red, ulcerated tissues extending to the throat and cheeks.
Unraveling the Root Causes
The exact etiology remains elusive, but evidence points to a hypersensitivity reaction. Plaque and tartar harbor pathogens that provoke the immune system abnormally. Viruses such as feline calicivirus or herpesvirus may prime cats for this response, while genetic predisposition plays a role in purebreds like Persians.
Unlike humans, cats rarely respond to antibiotics alone, underscoring it’s not purely infectious. Poor oral hygiene exacerbates it, but even diligent brushing fails in advanced stages.
Diagnostic Approaches for Accurate Confirmation
Veterinarians start with a physical exam under sedation for a thorough oral inspection. Key diagnostics include:
- Full-mouth radiographs to detect hidden abscesses or bone loss
- Biopsy of affected tissues to rule out cancer or autoimmune issues
- Bloodwork to assess overall health and infection markers
These steps differentiate stomatitis from resorptive lesions or tumors, ensuring targeted therapy.
Primary Treatment: Surgical Tooth Extractions
Dental extractions form the cornerstone of therapy, with partial or full-mouth removal proving most effective. Removing all premolars and molars (caudal mouth) succeeds in 70-80% of cases, while full extractions boost rates to 90-95% resolution.
Under general anesthesia, vets perform ultrasonic scaling, root removal, and alveoloplasty (smoothing bone sockets). Cats adapt remarkably, eating soft foods without issue post-healing. Studies confirm 67-80% achieve substantial improvement or cure.
| Extraction Type | Teeth Removed | Success Rate | Best For |
|---|---|---|---|
| Partial | Premolars & Molars | 70-80% | Milder cases |
| Full-Mouth | All teeth | 90-95% | Severe, refractory |
| Staged | Multiple sessions | Variable | High-risk cats |
Data synthesized from veterinary studies.
Supportive Medical Therapies
Pre- and post-surgery, multimodal pain control is vital: opioids, NSAIDs, and gabapentin manage discomfort. Broad-spectrum antibiotics curb secondary infections, while anti-inflammatories like corticosteroids offer short-term relief but aren’t curative long-term.
For refractory cases (10-30%), mesenchymal stem cell therapy shows promise, modulating immunity for remission where extractions fall short.
Home Care Strategies During Recovery
Post-op, transition to canned food softened with water for 2-4 weeks. Appetite stimulants like mirtazapine encourage eating if needed. Daily chlorhexidine rinses or gels maintain hygiene without brushing painful areas.
- Monitor for swelling or discharge; contact vet if persists
- Provide fresh water and elevated bowls for comfort
- Avoid hard treats or kibble until cleared
Healing timelines: extraction sites close in 2-4 weeks, inflammation subsides over 3-6 months, full benefits up to 2 years.
Long-Term Maintenance for Lasting Health
Many cats become medication-free post-extractions, but monitoring prevents flares. Annual vet checkups, dental radiographs, and soft diets sustain gains. Stress reduction via single-cat homes or pheromone diffusers aids immunity.
Dietary shifts to hypoallergenic or high-protein formulas may minimize triggers. Low-level laser therapy supports healing in some protocols.
Prognosis and Realistic Expectations
With prompt intervention, most cats regain appetite, groom normally, and enjoy extended lifespans. Refractory cases (under 20%) require lifelong low-dose meds or advanced options, but quality of life improves dramatically.
Early detection via routine exams prevents progression; owners report happier, heavier cats within months.
Frequently Asked Questions
Can cats live without teeth?
Yes, toothless cats thrive on wet or softened food, often gaining weight as pain resolves.
Is stomatitis contagious?
No, though underlying viruses like calicivirus spread between cats.
How much does treatment cost?
Expect $1,000-$3,000 for extractions, varying by case complexity and location.
Will my cat need pain meds forever?
Rarely; 90% discontinue after healing.
Can diet alone cure stomatitis?
No, but soft, anti-inflammatory foods support recovery.
Preventive Measures for Oral Wellness
Daily tooth brushing with enzymatic paste, dental diets, and water additives reduce plaque. Vaccinations against calicivirus lower risk. Spay/neuter may indirectly help via stress reduction.
Regular vet dental checks catch gingivitis before stomatitis develops.
References
- Gingivitis and Stomatitis in Cats — VCA Animal Hospitals. Accessed 2026. https://vcahospitals.com/know-your-pet/gingivitis-and-stomatitis-in-cats
- FCGS Treatment: New Hope for Cats with Chronic Mouth Pain — Veterinary Dentistry. Accessed 2026. https://veterinarydentistry.net/feline-chronic-gingivostomatitis-diagnosis-treatment/
- Managing Feline Stomatitis: Causes, Symptoms, and Treatments — PVDS. Accessed 2026. https://pvds.ca/treating-feline-stomatitis/
- Stomatitis in Cats: Symptoms, Causes and Treatment — PetMD. Accessed 2026. https://www.petmd.com/cat/conditions/mouth/stomatitis-in-cats
- 2025 FelineVMA Feline Oral Health and Dental Care Guidelines — PMC (Peer-reviewed). 2025. https://pmc.ncbi.nlm.nih.gov/articles/PMC12665832/
Read full bio of Sneha Tete