Canine Urinary Calculi: Formation, Recognition, and Management
Learn how mineral deposits develop in dogs' bladders and discover effective treatment approaches.
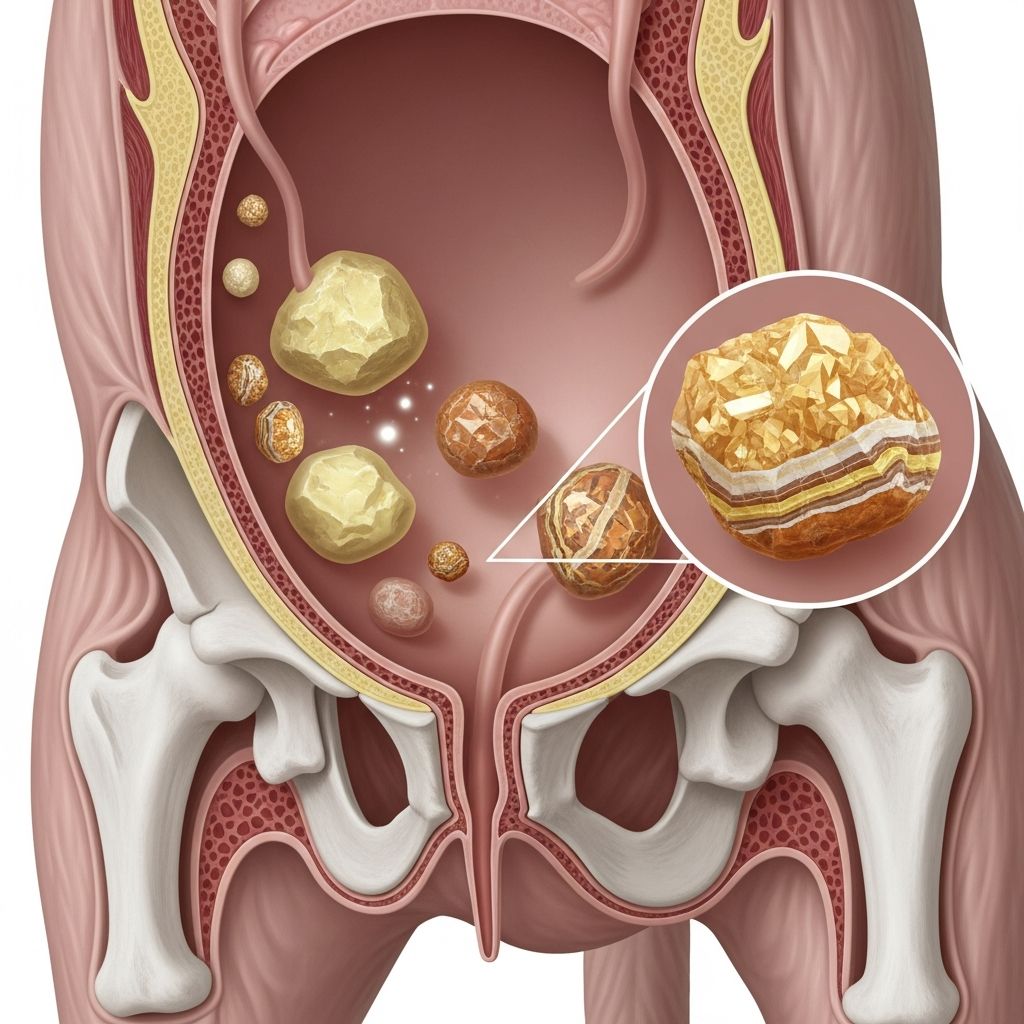
Bladder stones represent a significant health concern affecting numerous dogs across various age groups and breeds. These mineralized accumulations, clinically referred to as uroliths or urinary calculi, develop within a dog’s urinary bladder and can escalate into serious complications if not addressed promptly. Understanding the underlying mechanisms of stone formation, recognizing early warning indicators, and exploring available treatment pathways empowers dog owners to make informed decisions regarding their pet’s urinary health.
Understanding Mineral Deposits in Canine Urinary Systems
Bladder stones form through a complex interplay of physiological and environmental factors that remain incompletely understood by veterinary professionals. These mineralized deposits vary considerably in size, composition, and clinical significance. The formation process typically involves the accumulation of mineral compounds that crystallize within the bladder environment, creating solid structures that can range from microscopic particles to substantial masses requiring surgical intervention.
The composition of bladder stones determines their response to various treatment approaches. The most prevalent types encountered in veterinary practice include struvite stones (magnesium ammonium phosphate), calcium oxalate formations, and less common varieties such as urate, cystine, and silicate stones. Each stone type exhibits distinct characteristics regarding formation mechanisms, dissolution potential, and treatment requirements.
Primary Risk Factors Contributing to Stone Development
Multiple interconnected conditions increase a dog’s susceptibility to developing urinary calculi. Veterinary research has identified several key contributing factors:
- Urinary tract infections: These represent the most prevalent predisposing cause, as bacterial colonization alters urine pH levels and promotes mineral crystallization
- Dehydration and infrequent urination: Reduced fluid intake and prolonged intervals between micturition allow mineral-laden urine to concentrate within the bladder, increasing stone formation probability
- Dietary composition: Excessive levels of magnesium, phosphorus, and protein in commercial pet foods contribute significantly to stone formation, particularly struvite types
- Urine pH imbalances: Alkaline urine environments favor struvite crystallization, while acidic conditions promote calcium oxalate precipitation
- Genetic predisposition: Certain dog breeds exhibit inherited metabolic abnormalities that increase urinary stone risk
- Urinary stagnation: Incomplete bladder emptying or prolonged urine retention allows crystal formation and bacterial proliferation
Additionally, environmental factors including climate and lifestyle patterns may influence stone development. Dogs residing in arid regions with naturally lower water availability face elevated dehydration risks, particularly if water intake remains insufficient.
Recognizing Clinical Manifestations
Dogs experiencing bladder stone complications typically display distinctive urinary and behavioral changes. Early recognition of these signs enables prompt veterinary intervention before serious complications develop.
Primary urinary symptoms include:
- Blood in urine (hematuria), often accompanied by pink or red discoloration
- Straining during urination (dysuria) with production of minimal urine volumes
- Dramatic increase in urination frequency and urgency (pollakiuria)
- Visible discomfort or vocalization during micturition
- Cloudiness or unusual discoloration of urine
Secondary manifestations may encompass:
- Licking or excessive attention to genital region due to inflammation
- Abdominal pain and tenderness, particularly in lower abdominal regions
- Loss of appetite and progressive weight loss
- Behavioral changes including increased restlessness or agitation
- Lethargy and reluctance to engage in normal physical activities
- Reluctance to jump or climb stairs
Male dogs encounter particularly severe complications due to their anatomically longer and narrower urethra. Small stones can migrate into the urethra and lodge, creating partial or complete obstructions that prevent urination. Complete urinary obstruction represents a life-threatening emergency requiring immediate veterinary intervention.
Pathophysiological Mechanisms of Stone-Related Irritation
Bladder stones cause clinical symptoms through multiple mechanical and inflammatory pathways. The solid mineral surfaces physically abrade the delicate bladder lining as the organ contracts during normal function. This constant irritation damages the protective urothelial tissue, resulting in inflammation, bleeding, and pain sensation.
Inflammation of the bladder wall (cystitis) leads to muscle spasms and increased contractility, which manifests as straining and urinary urgency. Stones positioning themselves at the bladder neck—the anatomical junction connecting the bladder to the urethra—can function similarly to a valve, obstructing urine flow and creating additional pain and straining sensations.
Diagnostic Approaches and Confirmation Methods
Veterinary professionals employ multiple diagnostic techniques to confirm bladder stone presence and determine stone composition:
- Urinalysis: Microscopic examination reveals crystal formation, abnormal pH levels, and signs of infection
- Radiographic imaging: X-ray examination visualizes radiopaque stones; ultrasound detects all stone types regardless of mineral composition
- Urine culture: Bacterial identification guides appropriate antimicrobial selection
- Stone analysis: Evaluation of surgically or naturally passed stones determines precise composition and guides prevention strategies
Comparative Treatment Modalities
| Treatment Approach | Best For | Advantages | Limitations |
|---|---|---|---|
| Dietary Dissolution | Struvite stones; small non-obstructing stones | Non-invasive; avoids surgical risks; typically costs less | Requires weeks to months; unsuitable for calcium oxalate stones; requires strict dietary compliance |
| Medical Flushing | Small bladder stones | Minimally invasive; avoids general anesthesia | Limited effectiveness with larger stones; may require multiple procedures |
| Laser Lithotripsy | Large stones difficult to remove surgically | Breaks stones into smaller fragments; allows natural passage | Specialized equipment required; not universally available |
| Surgical Removal | Large or multiple stones; obstructive cases; calcium oxalate stones | Fastest resolution; immediately relieves symptoms; definitive treatment | Requires general anesthesia; involves surgical recovery period |
Medical Dissolution Protocols for Struvite Calculi
Struvite stones represent the only bladder stone type amenable to medical dissolution therapy. This treatment approach fundamentally alters urine chemistry to create conditions unfavorable to stone continuation.
Therapeutic diets specifically formulated for struvite dissolution contain reduced magnesium, phosphorus, and protein concentrations while simultaneously promoting urinary acidification and dilution. These formulations work through multiple mechanisms:
- Creating undersaturated urine conditions that prevent crystal formation and cause existing stones to gradually dissolve
- Increasing sodium content to stimulate drinking and enhance urinary output, promoting mechanical stone flushing
- Acidifying urine pH to shift the chemical environment away from struvite precipitation
- Lowering mineral concentrations to reduce available stone-forming substrates
Commonly prescribed therapeutic diets include Hill’s Prescription Diet C/D, Royal Canin Urinary SO, and Purina Pro Plan UR formulations. Clinical experience demonstrates that struvite stone dissolution typically progresses over 8-12 weeks, though symptom relief often occurs within the initial treatment period.
The dissolution rate correlates directly with stone surface area exposure to undersaturated urine and concurrent control of any urinary tract infections. Bacterial involvement slows the dissolution process; therefore, concurrent antibiotic therapy frequently accompanies dietary dissolution protocols.
Surgical Intervention for Obstructive and Calcium Oxalate Stones
Surgical removal remains the most efficient treatment option for numerous stone types and clinical presentations. The standard surgical procedure, termed cystotomy, involves creating an incision through the bladder wall to directly access and remove accumulated stones.
This approach proves particularly essential for:
- Calcium oxalate, urate, cystine, and silicate stones that cannot dissolve through dietary management
- Dogs presenting with urinary obstruction requiring immediate treatment
- Situations where general anesthesia risk is acceptable compared to potential complications from prolonged stone presence
- Dogs with multiple large stones unsuitable for passage through the urethra
Cystotomy represents a routine surgical procedure in veterinary practice, with most dogs achieving rapid postoperative recovery. The procedure provides immediate symptom relief and prevents stone-related complications from progressing further.
Advanced Non-Surgical Removal Techniques
Alternative approaches to traditional surgery offer effective options for selected cases. Urohydropropulsion involves strategically flushing the bladder using saline solution via urinary catheter to encourage stone passage through the urethra. This technique succeeds most effectively with smaller stones and dogs lacking complete urinary obstruction.
Laser lithotripsy represents an increasingly available procedure that uses focused laser energy to fragment large bladder stones into smaller pieces compatible with natural urinary passage. This technology proves particularly valuable for dogs with extensive stone burden unsuitable for traditional surgical removal.
Comprehensive Disease Management and Prevention Strategies
Regardless of the primary treatment selected, concurrent management of predisposing conditions significantly impacts outcomes and recurrence rates. Urinary tract infections require identification and appropriate antibiotic therapy to prevent future stone formation.
Long-term prevention focuses on modifying risk factors:
- Dietary optimization: Transition to formulations maintaining appropriate mineral balance and urinary pH
- Hydration enhancement: Encourage increased water consumption through multiple water sources, elevated bowls, or water fountains
- Urinary frequency: Provide frequent opportunities for micturition to prevent urine stagnation
- Monitoring: Schedule regular veterinary check-ups with periodic urinalysis to detect crystal formation early
- Medication compliance: Continue prescribed antibiotics or urinary acidifying agents as directed
Frequently Asked Questions About Canine Bladder Stones
- Can all bladder stones be dissolved through diet?
- No. Only struvite stones respond reliably to dietary dissolution protocols. Calcium oxalate and other stone types require either surgical removal or advanced technologies like laser lithotripsy.
- How quickly does surgical treatment provide relief?
- Surgical cystotomy eliminates stones immediately, with symptom relief occurring within hours to days post-recovery. Dietary dissolution requires weeks to months for stone resolution.
- Does neutering or spaying influence bladder stone development?
- Some research suggests spayed female dogs may face slightly elevated stone risk due to hormonal influences on urinary pH and mineral metabolism, though this remains an area requiring further investigation.
- Can bladder stones recur after successful treatment?
- Recurrence remains possible without ongoing preventive measures. Maintaining appropriate diet, hydration, and regular veterinary monitoring substantially reduces recurrence probability.
- Are certain dog breeds predisposed to bladder stones?
- Yes. Specific breeds exhibit increased genetic susceptibility to stone formation. Dalmatians face elevated urate stone risk, while Miniature Schnauzers, Bichon Frises, and others show increased struvite stone incidence.
Conclusion: Empowering Dog Owners Through Knowledge
Bladder stones represent a manageable health challenge when recognized early and addressed appropriately. Understanding the multifactorial nature of stone formation, recognizing clinical indicators, and working collaboratively with veterinary professionals ensures optimal outcomes for affected dogs. With multiple effective treatment approaches available and evidence-based prevention strategies established, dogs affected by urinary calculi can return to normal, comfortable, and active lives.
References
- Bladder Stones in Dogs: Causes, Symptoms, & Treatment — Long Beach Animal Hospital. Accessed March 2026. https://lbah.com/canine/dog-bladder-stones/
- Understanding Bladder Stones in Dogs: Causes, Symptoms, and Treatment — HVS Veterinary. Accessed March 2026. https://www.hvsevet.com/blog/25/understanding-bladder-stones-in-dogs-causes-symptoms-and-treatment
- Bladder Stones in Dogs: Causes, Symptoms and Treatments — CareCredit. Accessed March 2026. https://www.carecredit.com/well-u/pet-care/bladder-stones-dogs/
- Bladder Stones in Dogs: Symptoms, Prevention, and More — PetMD. Accessed March 2026. https://www.petmd.com/dog/conditions/urinary/bladder-stones-dogs-symptoms-prevention-and-more
- Struvite bladder stones in dogs — Cornell University College of Veterinary Medicine, Riney Canine Health Center. Accessed March 2026. https://www.vet.cornell.edu/departments-centers-and-institutes/riney-canine-health-center/canine-health-topics/struvite-bladder-stones-dogs
- Bladder Stones in Dogs — VCA Animal Hospitals. Accessed March 2026. https://vcahospitals.com/know-your-pet/bladder-stones-in-dogs
- Bladder Stones in Dogs: Causes, Symptoms, Prevention, and Treatment — Bliss Animal Hospital, Orange County. Accessed March 2026. https://blissanimalhospital.com/blog/bladder-stones-in-dogs-orange-county/
- Bladder Stones in Dogs — Small Door Veterinary. Accessed March 2026. https://www.smalldoorvet.com/learning-center/medical/bladder-stones-in-dogs
Read full bio of medha deb